Table of Contents
The Early Days of HIV
HIV was first identified in the early 1980s, and it quickly became clear that the virus was responsible for a new, devastating disease: Acquired Immunodeficiency Syndrome (AIDS). At the time, little was known about the virus, its transmission, or how to treat it. Patients diagnosed with AIDS were often given a death sentence, as the disease severely weakened the immune system, leaving individuals vulnerable to opportunistic infections and cancers.
In the early years of the epidemic, treatment options were virtually nonexistent, and the public health response was marked by fear, stigma, and a lack of understanding. Despite the widespread panic, early HIV activists and doctors began to push for better research, more funding, and a greater focus on treatment options.

The turning point in the battle against HIV came with the development of antiretroviral therapy (ART) in the mid-1990s. ART is a combination of drugs that target different stages of the HIV life cycle, preventing the virus from replicating and allowing the immune system to rebuild. These therapies do not cure HIV but, when taken consistently, can reduce the viral load to undetectable levels. This means that HIV can be controlled with proper medication, and individuals can live a normal lifespan.
One of the most important aspects of ART is its ability to lower the viral load to undetectable levels. An undetectable viral load means that the virus cannot be transmitted through sexual contact—a concept known as “undetectable = untransmittable” (U=U). This has significantly reduced the stigma associated with HIV and allowed people with HIV to lead full, healthy lives.
The introduction of ART was groundbreaking. The cocktail of drugs provided an effective means of controlling HIV, and it was quickly adopted as the gold standard for treatment. Since then, there have been numerous improvements in ART, with newer medications offering fewer side effects, greater convenience (e.g., one-pill regimens), and more effective viral suppression.
From Terminal to Chronic
Before ART, HIV was considered an acute, terminal illness. The progression from HIV to AIDS was inevitable without effective treatment. But with ART, the disease has shifted from a terminal diagnosis to a manageable chronic condition, much like diabetes or hypertension. People with HIV who adhere to ART can live as long as those without the virus, provided they continue treatment and manage their health effectively.
The shift in perspective has been transformative not only for people living with HIV but also for healthcare systems. Once seen as a death sentence, HIV is now managed through a lifelong treatment regimen. This new understanding has had profound implications for public health, social acceptance, and research funding.
Scientific Advancements
While ART has made HIV a manageable condition, the ultimate goal remains the eradication of the virus. For years, scientists have been working on finding a cure for HIV, and significant progress has been made. One avenue of research is focused on a “functional cure,” which aims to achieve long-term viral suppression without the need for ongoing ART.
In recent years, there have been promising breakthroughs in gene therapy and immunotherapy. For example, the “Berlin Patient” and the “London Patient” are two individuals who, after receiving stem cell transplants, have shown no detectable trace of HIV in their systems. While these cases are extraordinary and not yet replicable on a wide scale, they offer hope that a cure may one day be possible.
Researchers are also exploring “kick and kill” strategies, which involve activating latent HIV reservoirs in the body and then eliminating the virus. Although these approaches are still in early stages, they demonstrate that finding a cure for HIV is within reach.
Pre-Exposure Prophylaxis (PrEP)
In addition to treatment, prevention efforts have played a crucial role in reducing the spread of HIV. One of the most effective tools for HIV prevention is pre-exposure prophylaxis (PrEP), a medication taken by HIV-negative individuals to reduce the risk of acquiring HIV. PrEP has been shown to be highly effective when taken consistently, reducing the risk of HIV transmission by up to 99%.
PrEP has been a game-changer, particularly for high-risk populations, such as men who have sex with men, individuals in serodiscordant relationships (where one partner is HIV-positive and the other is HIV-negative), and people who inject drugs. By preventing the transmission of HIV in the first place, PrEP has become a vital part of global HIV prevention strategies.
Reducing Stigma and Access to Care
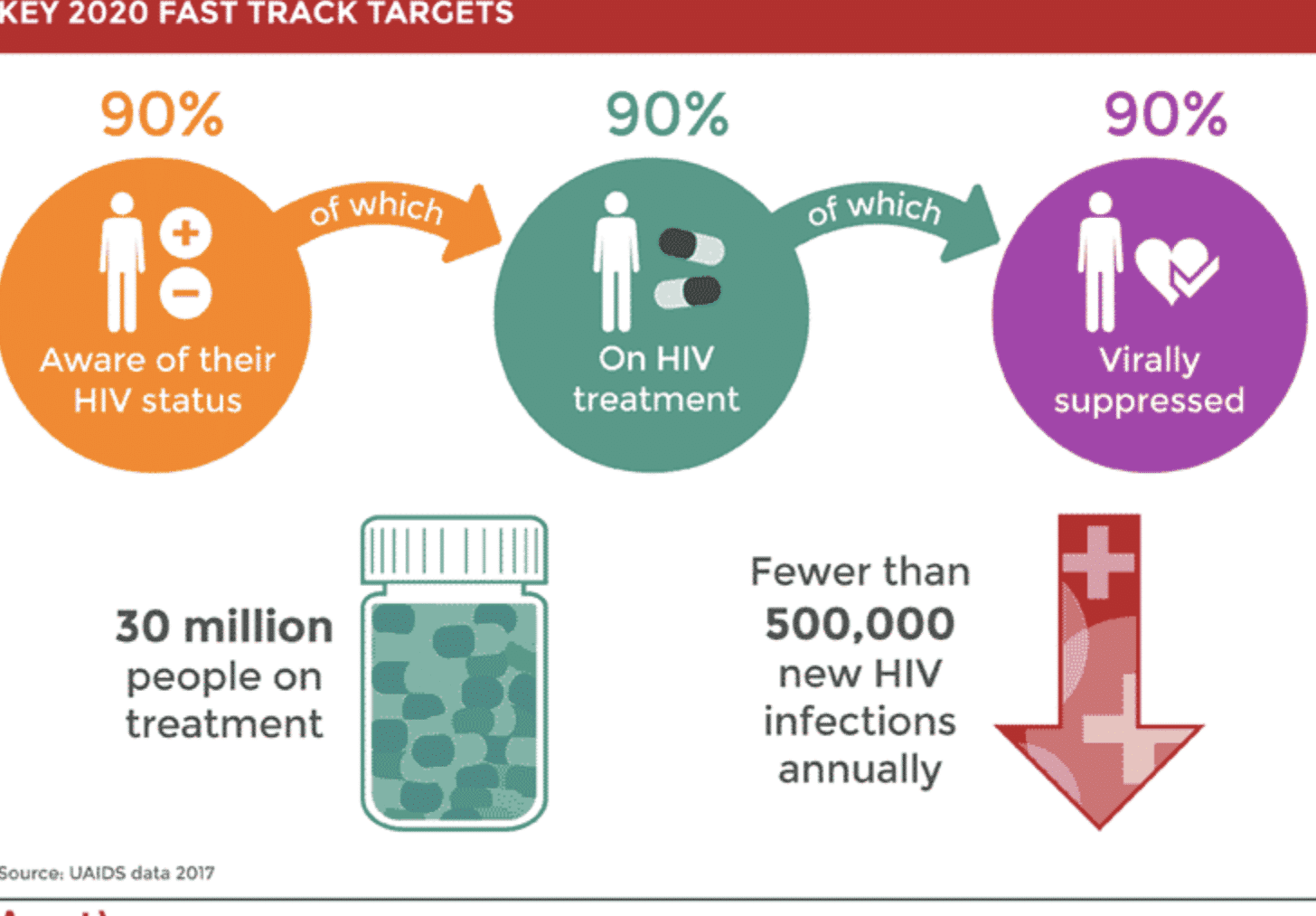
The widespread availability of ART and prevention strategies like PrEP has had a profound impact on global HIV rates. According to the World Health Organization (WHO), more than 38 million people worldwide are living with HIV, but with continued advancements in treatment and prevention, millions more are living healthier lives.
However, despite the progress, stigma remains one of the most significant barriers to effective HIV treatment and prevention. Many people with HIV continue to face discrimination, which can prevent them from seeking care or adhering to their treatment regimens. Global efforts to reduce HIV-related stigma are essential to ensuring that all individuals have access to the care and support they need.
In many regions, particularly in low- and middle-income countries, access to ART and prevention tools is still limited. Global organizations, including the WHO and UNAIDS, are working to expand access to these life-saving interventions, with the ultimate goal of ending the HIV epidemic by 2030.
Towards an End to the HIV Epidemic
Looking forward, the ultimate goal is not just to treat HIV but to end the epidemic altogether. The path to ending HIV will require continued advancements in treatment, prevention, and ultimately a cure. It will also require a global commitment to reducing stigma, increasing access to care, and ensuring that people living with HIV have the support they need to thrive.
As science continues to evolve, there is hope that HIV will no longer be a public health threat in the future. In the meantime, ART and PrEP continue to offer hope to millions of people worldwide, allowing them to live long, healthy lives free from the fear of a terminal diagnosis.
A New Era of Hope
HIV is no longer a terminal illness. Thanks to advancements in treatment and prevention, people with HIV can live long, fulfilling lives. While the fight for a cure continues, the medical community has made tremendous progress in controlling the virus, making it a chronic but manageable condition. The journey from death sentence to manageable illness is a remarkable achievement, but the work is not over. With continued research and global cooperation, the goal of ending the HIV epidemic by 2030 is within reach.