At first, the differences appeared subtle. A slight narrowing of the lower face. A softer jawline. Cheeks that no longer held their original contour. But over time, patterns emerged that told a deeper story. Missing teeth were not just a cosmetic concern or a functional inconvenience. They were triggering a biological chain reaction that reshaped the jawbone itself, altering facial structure, accelerating visible aging, and affecting overall health in ways many patients never anticipated.
For decades, tooth loss was often framed as an isolated dental issue. Replace the tooth, restore the bite, move on. But modern dentistry and imaging technology have revealed that the mouth is not a standalone system. It is deeply connected to bone health, facial symmetry, posture, and even long-term systemic wellbeing.
Table of Contents
- Tooth roots do more than hold teeth in place.
- Bone loss begins sooner than most people realize.
- As the jawbone shrinks, the face begins to change.
- The impact extends beyond appearance.
- Why dentures alone do not stop bone loss.
- Dental implants changed how dentists approach tooth loss.
- The psychological effects are often overlooked.
- Aging and tooth loss are not the same process.
- Prevention starts earlier than most expect.
- The mouth reflects the body’s broader health systems.
- Technology is making invisible changes visible.
- What this means for the future of dental care.
- In the end, missing teeth are not just about what’s gone.
Tooth roots do more than hold teeth in place.
Healthy teeth are anchored into the jawbone through roots that play a crucial biological role. Every time a person chews, bites, or speaks, mechanical forces travel through the tooth roots into the jawbone. These forces stimulate bone cells, signaling the body to maintain bone density in that area.
This process is known as bone remodeling. It is the same principle that keeps leg bones strong when people walk or lift weights. The jawbone, like all bones, depends on regular stimulation to remain dense and healthy.
When a tooth is lost, that stimulation disappears almost immediately.
Bone loss begins sooner than most people realize.
Once a tooth is missing, the section of jawbone that once supported it no longer receives mechanical input. The body, efficient and adaptive, begins to interpret that bone as unnecessary. Gradually, it starts to resorb the bone tissue.
Studies in dentistry show that jawbone loss can begin within months of tooth extraction. In the first year alone, patients may lose a significant percentage of bone volume in the affected area. Over time, this bone loss continues, often silently, without pain or obvious warning signs.
This is why missing teeth are often described by dentists as a progressive condition rather than a static one.
As the jawbone shrinks, the face begins to change.
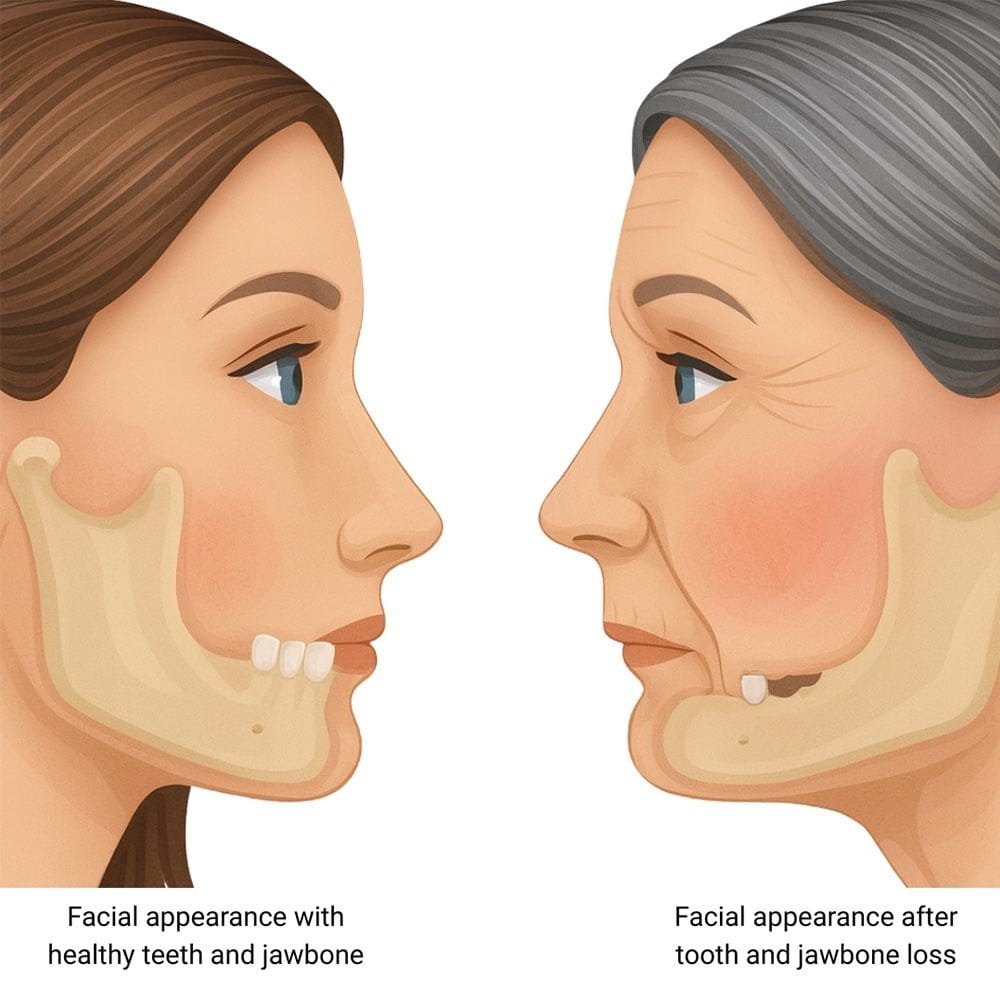
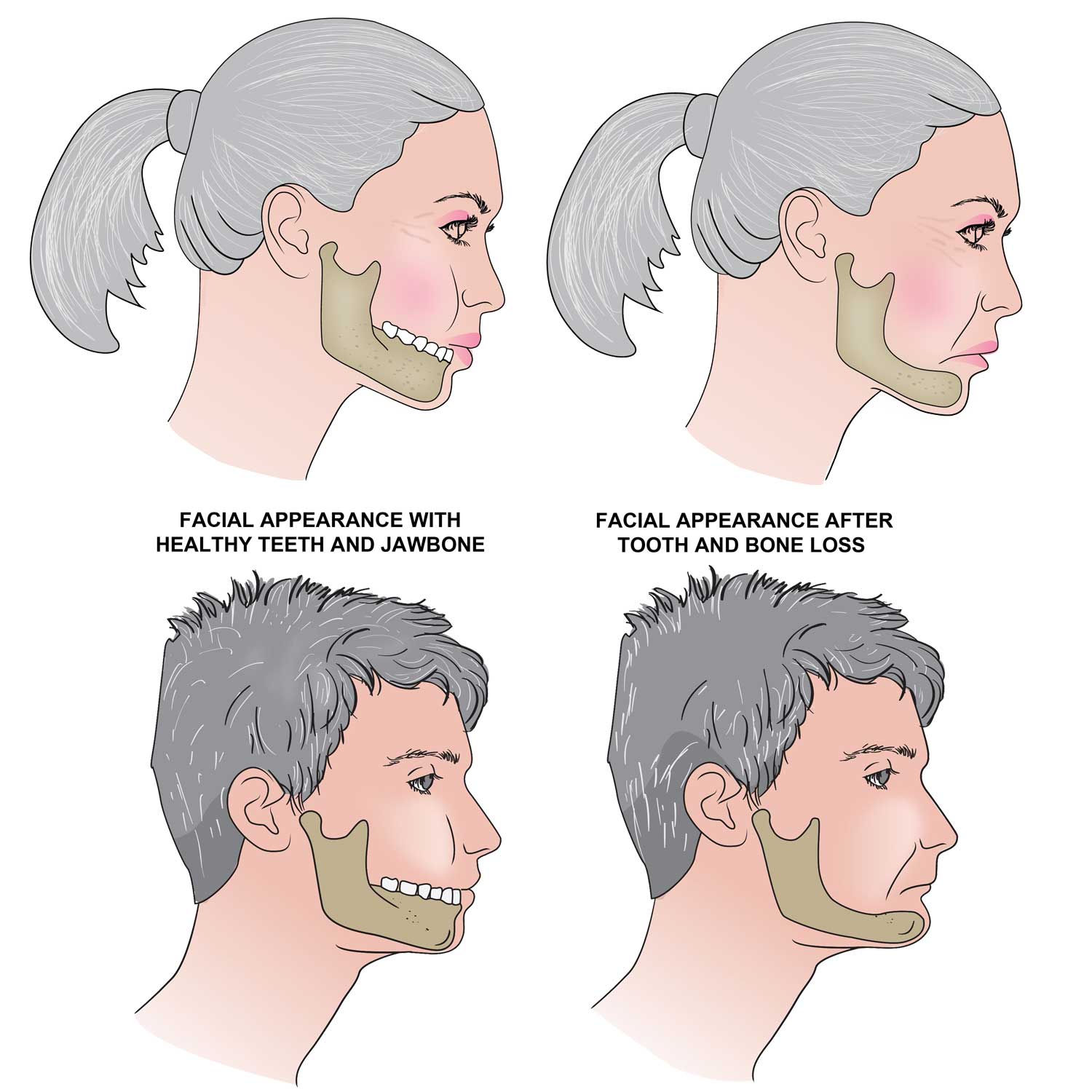
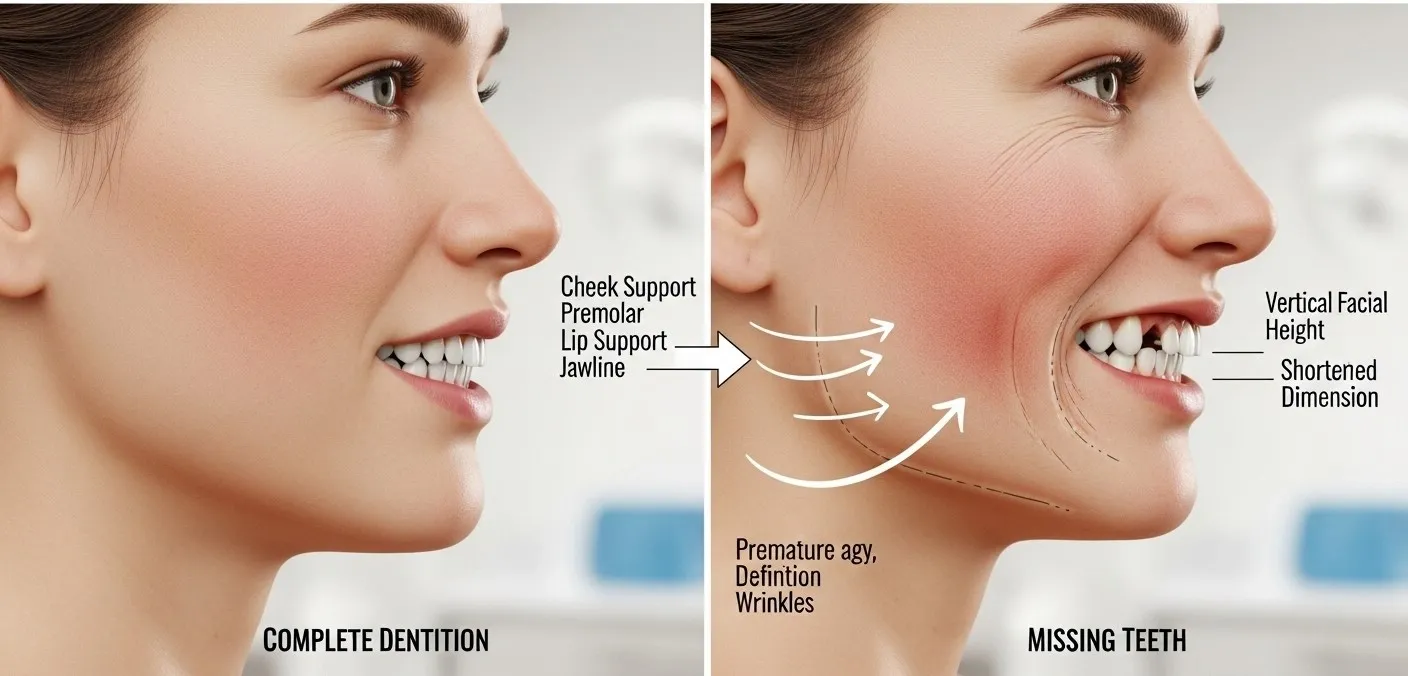
The jawbone serves as the structural foundation of the lower face. It supports the lips, cheeks, and muscles that give the face its shape. When bone volume decreases, the soft tissues above it lose their support.
This leads to visible changes that many people mistakenly attribute solely to aging. Lips appear thinner. The chin may move closer to the nose. Deep lines form around the mouth. The lower third of the face shortens, creating a collapsed appearance.
Dentists often refer to this as facial collapse, and it can significantly alter a person’s appearance over time. What surprises many patients is how closely these changes track with untreated tooth loss rather than chronological age alone.
The impact extends beyond appearance.
Jawbone deterioration affects more than facial aesthetics. As the bone recedes, it alters how remaining teeth align and function. Neighboring teeth may begin to shift into empty spaces, disrupting the bite and placing uneven stress on the jaw joint.
This imbalance can contribute to temporomandibular joint discomfort, headaches, and chronic muscle tension in the face and neck. Chewing efficiency decreases, often leading people to avoid certain foods, which can affect nutrition.
Speech patterns may subtly change as well. Teeth play a role in articulation, and their absence can influence how sounds are formed, especially over time as the jaw structure adapts to the loss.
Why dentures alone do not stop bone loss.
Traditional dentures restore the appearance of teeth, but they do not address the underlying biological problem. Dentures sit on top of the gums rather than integrating with the jawbone. As a result, they do not provide the stimulation necessary to preserve bone density.
In fact, prolonged denture use without bone support can sometimes accelerate bone loss by placing pressure on already resorbing bone. This explains why dentures often become loose over time, requiring repeated adjustments.
Modern dentistry increasingly emphasizes solutions that interact with the jawbone itself, rather than simply replacing the visible tooth.
Dental implants changed how dentists approach tooth loss.
Dental implants are designed to function like natural tooth roots. Surgically placed into the jawbone, they provide the mechanical stimulation needed to maintain bone density. When integrated properly, implants can halt bone loss in the area and preserve facial structure.
This shift in treatment philosophy reflects a broader understanding of oral health as skeletal health. Dentists now evaluate not just teeth, but the long-term stability of the jawbone and face.
Early intervention matters. The longer bone loss progresses, the more complex restoration becomes.
The psychological effects are often overlooked.
Beyond physical changes, tooth loss can carry emotional consequences. As facial structure changes, many individuals experience a decline in self-confidence. They may avoid smiling, social situations, or photographs.
These behavioral changes can quietly affect mental health, reinforcing isolation and self-consciousness. What begins as a dental issue can ripple outward into daily life in unexpected ways.
Recognizing these effects has prompted a more holistic approach in dentistry, one that considers emotional wellbeing alongside physical outcomes.
Aging and tooth loss are not the same process.
A common misconception is that facial changes caused by tooth loss are simply part of natural aging. While aging does influence skin elasticity and muscle tone, the rapid structural changes associated with jawbone resorption are distinct.
Dentists can often distinguish between age-related changes and those caused by bone loss by examining facial proportions. Patients who have maintained their teeth tend to retain stronger jaw definition longer than those who experience early tooth loss.
This distinction underscores the role of oral health in overall aging patterns.
Prevention starts earlier than most expect.
Maintaining jawbone health begins long before teeth are lost. Regular dental checkups, early treatment of gum disease, and addressing damaged teeth promptly all contribute to preserving bone structure.
When extractions are unavoidable, dentists increasingly discuss bone-preserving options immediately. Timing matters. Interventions performed soon after tooth loss are more effective at preventing long-term damage.
Education plays a critical role here. Many patients are unaware that delaying treatment can limit future options.
The mouth reflects the body’s broader health systems.
Emerging research continues to link oral health with systemic conditions such as cardiovascular disease, diabetes, and osteoporosis. Jawbone loss can sometimes mirror bone density changes elsewhere in the body.
Dentists often collaborate with physicians to identify underlying conditions that may contribute to rapid bone resorption. In this way, dental observations can become early indicators of broader health issues.
This interconnected perspective is reshaping how healthcare professionals view the mouth — not as a separate entity, but as part of a complex biological network.
Technology is making invisible changes visible.
Advanced imaging techniques, such as 3D scans and digital modeling, now allow dentists to track jawbone changes with remarkable precision. Patients can see side-by-side comparisons of their facial structure over time.
This visual evidence often changes how people perceive tooth loss. What once seemed like a minor inconvenience becomes a tangible, preventable process with long-term consequences.
Awareness, in many cases, becomes the turning point.
What this means for the future of dental care.
The growing understanding of how missing teeth affect the jaw and face is driving a shift toward preventative, bone-focused dentistry. Treatment plans increasingly emphasize preserving structure rather than reacting to damage after it occurs.
As research advances, solutions are becoming more accessible, more precise, and more personalized. Dentists are no longer simply restoring smiles; they are preserving faces, function, and quality of life.
In the end, missing teeth are not just about what’s gone.
They are about what quietly changes in their absence. Bone resorbs. Faces adapt. Function shifts. And often, people do not realize what is happening until the transformation is well underway.
Understanding this process empowers individuals to make informed decisions earlier, when prevention is still possible and outcomes are more predictable.
The jawbone remembers every tooth that once supported it. And when that support disappears, the consequences unfold slowly, invisibly, and relentlessly — unless action is taken.