
Imagine sitting in a clinic, getting a routine mammogram—and being told, “We’ve spotted changes that might lead to cancer in the next three to five years.”
It sounds like science fiction, but thanks to the team at Massachusetts Institute of Technology (MIT), it’s becoming reality. Researchers have developed an AI-powered model that predicts the risk of breast cancer well before any symptoms appear.
This is not just about health—it’s about shifting how we spend on medical screening, how insurers price risk, how hospitals invest in technology, and how women plan their lives. The ripple touches health, finance, technology—and your future.
Let’s pull back the curtain.
Table of Contents
The research breakthrough: meeting “Mirai”
The AI model, named Mirai, developed by MIT’s CSAIL and Jameel Clinic, is built to analyze mammograms alongside clinical risk factors like age, family history, and breast density.
What makes Mirai powerful?
- It was trained on over 200,000 mammogram exams from Massachusetts General Hospital (MGH).
- It was validated across different populations and hospitals—including Sweden and Taiwan—ensuring it works not just for one demographic.
- It predicts risk across multiple future time-points (e.g., 2-year risk vs 5-year risk) rather than just “will you have cancer or not.”
- It holds accuracy across racial groups, breast densities and cancer subtypes—a major win for health equity.
If this were in your inbox, what would you do with the chance to know your risk ahead of time?
Why this matters: from scanning rooms to your wallet
Let’s step out of the lab and into the wider world. Because this isn’t just about catching cancer—it’s about money, decision-making and prevention economics.
Screening costs and health-finance implications
Traditional risk-models rely on family history or age, but their predictive power is limited. Mirai outperforms classic methods (such as the Tyrer-Cuzick model) by identifying nearly twice as many future cancers.
That means: fewer late-stage treatments (which cost more), fewer unnecessary scans for low-risk people, and smarter allocation of healthcare resources.
Personalized screening: free up resources
With Mirai’s risk estimates, doctors could tailor screening schedules. A woman flagged as high-risk might be screened more often; a lower-risk woman might avoid unnecessary mammograms for a period.
That saves money—on your side and on the system’s side—and reduces anxiety, radiation exposure, and false positives.
Investment in tech and workflow
Hospitals implementing this kind of AI need new hardware, data systems, staff training, and compliance workflows. That’s capital-intensive.
As a result, screening centers may charge more, insurers may change premiums, and patients could see tech-driven cost shifts in the “health-finance” chain.
And here’s a loop to keep you thinking: if your risk is flagged high, do you spring into action or resist the anxiety of being told “maybe you’ll get cancer”?
The health impact: catch it before it catches you
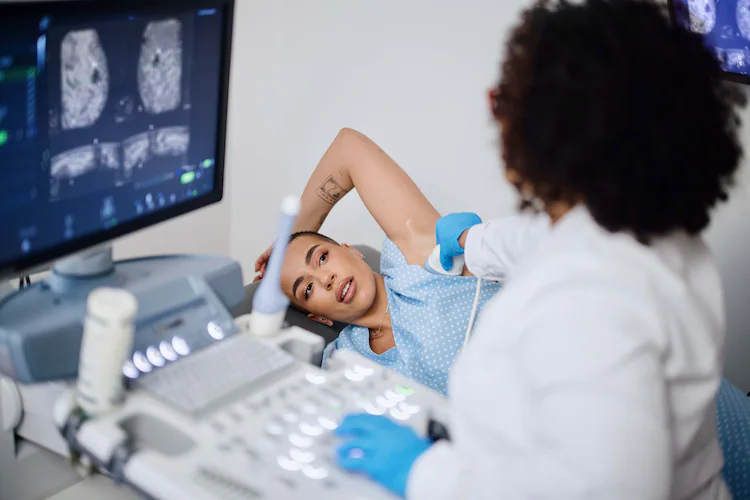
The heart of this story is health—because even the best finance or tech innovation counts only if it improves lives.
Early detection = better outcomes
Detecting cancer sooner means less aggressive treatment, more options, and often better survival. That’s a widely accepted fact.
But what if you could detect risk before the cancer actually develops? That changes the game from reactive to proactive. The article reports that Mirai could predict the likelihood of cancer years before symptoms appear.
Equity in screening
Historically, many risk-models under-predicted risk for non-white women, leading to disparities. Mirai’s performance is consistent across races and breast densities—helping bridge a major gap in preventive health.
For you, this means a smoother path to screening that fits your individual risk, not just “women over 50” or “dense breast” check-lists.
The evolving tech side
The researchers are now extending the model by using full imaging history and advanced modalities like tomosynthesis.
That means smarter scans, deeper insights—and eventually possibly less frequent screening for those at low risk.
If you put yourself in that future scanning chair—how would you want the machine to talk to you? “You’re safe for now” or “We’ve flagged you high risk—act now”?
How this changes your behaviour: what to ask and what to do
Because innovations are only useful if they create action. Let’s talk about how you, your family or your clinic can respond.
Ask the right questions
- Does the mammogram centre/clinic use an AI risk-prediction model?
- Are you being screened according to blanket guidelines or personalized risk?
- What’s your follow-up plan if you’re flagged high risk?
- What are the costs (financial and health) of extra screening or monitoring?
Stay in control of your health-finance
If you’re flagged as high risk:
- Consider lifestyle adjustments (exercise, diet, alcohol intake) that reduce cancer risk
- Ask about more sensitive imaging (MRI, tomosynthesis)
- Factor in costs of more frequent screening—insurance, time, travel.
If you’re flagged as low risk:
- Ask your provider how often you really need screening
- Use saved funds or time for other health-boosting investments.
Make tech literacy your advantage
Understanding the tech behind your screening helps you ask smarter questions. AI tools like Mirai aren’t perfect—they’re predictions, not certainties.
Make sure your clinician still interprets results in context.
And remember: this isn’t a plug-and-play for every patient yet—but it’s coming.
What’s next and where the ripple goes
This breakthrough is not the endpoint—it’s a launch pad. Here’s what’s coming—and why you should care.
Regulatory and ethical questions
Who owns your imaging data? How is AI trained and validated for your demographic? If an AI flags high risk, how does that affect insurance underwriting?
These are big finance and health questions that will shape how widely and affordably this tech is adopted.
Global accessibility
So far the model has been validated in multiple countries—but rolling it out globally, especially in low-resource settings, has challenges: imaging equipment, data infrastructure, training.
If you live outside a major city—will you have access to this next-gen screening? The inequality gap might shift rather than shrink.
Cost-benefit for the masses
Will insurers cover AI-augmented screening? Will you pay extra? Will you save money? The future of “health finance + prevention” depends on whether payers and providers buy in.
And if you’re reading this: how much would you pay for five-year peace of mind?
The tech arms-race
As AI models proliferate, expect competition: AI that predicts other cancers, other diseases, multi-modality imaging combined with genomics, wearable data.
The cost of prevention might go down—or it might dramatically increase.
And if you want even deeper coverage: what happens when your smartphone camera becomes a health-predictor?
What will you choose?
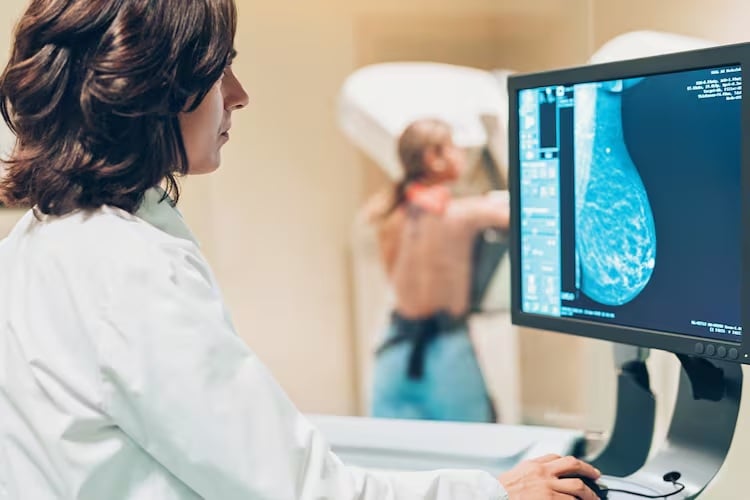
Here’s the personal question: if offered a mammogram with this AI predictive layer today, would you take it?
Would you want to know you have a 40 % risk five years out, so you invest now—and possibly spare surgery, chemo, late-stage treatment?
Or would you prefer the standard screening, no “what-ifs”, no anxiety from prediction?
By reading this, you’re part of the conversation. Because the tech is no longer in the lab—it’s walking into clinics, insurance boards, and your health-finance decisions.
Make no mistake: this is health and wealth. Prevention and cost-control. Fate and choice.