Table of Contents
- The review that reframed the GLP-1 conversation
- Why the 60% figure captured so much attention
- What the study actually looked at
- Why GLP-1 drugs work so well in the first place
- The part patients may find most discouraging
- Could tapering help reduce regain
- Why lifestyle support still matters
- What this means for the future of obesity care
The review that reframed the GLP-1 conversation
The new paper, published in eClinicalMedicine, did not focus on whether GLP-1 drugs can help people lose weight. That question has already been answered many times. Instead, it focused on what happens after those medications are discontinued. The researchers concluded that weight consistently rebounded after cessation of GLP-1 receptor agonists, with the steepest regain occurring in the months after treatment stopped. By 52 weeks, the model estimated that about 60% of the original weight loss had returned, and by around 60 weeks the regain began to plateau, with a projected long term regain of roughly 75% of the original loss. In practical terms, that means many patients may still keep off about one quarter of the weight they lost, but most of the initial benefit may diminish without an effective maintenance plan.
That is a striking conclusion, but it is also more nuanced than many viral headlines suggest. The same University of Cambridge summary emphasized that even after this rebound, an estimated 25% of the original weight loss may be sustained in the long term. For someone who lost 20% of their body weight while taking the medication, that could still translate to around a 5% sustained reduction from their starting weight. Researchers and commentators stressed that this is not medically trivial. In fact, even modest long term weight reduction can improve blood sugar, blood pressure, and cardiovascular risk.
So the real lesson of the review is not that GLP-1 medications fail. It is that obesity treatment behaves much more like chronic disease management than a short burst cure. That may sound obvious to specialists, but it cuts against how many people instinctively view weight loss. There is still a lingering belief that a successful treatment should end with a patient simply maintaining results on their own. The new review suggests that for many patients, the biology driving weight regain remains active even after a successful period of medication assisted loss.
Why the 60% figure captured so much attention
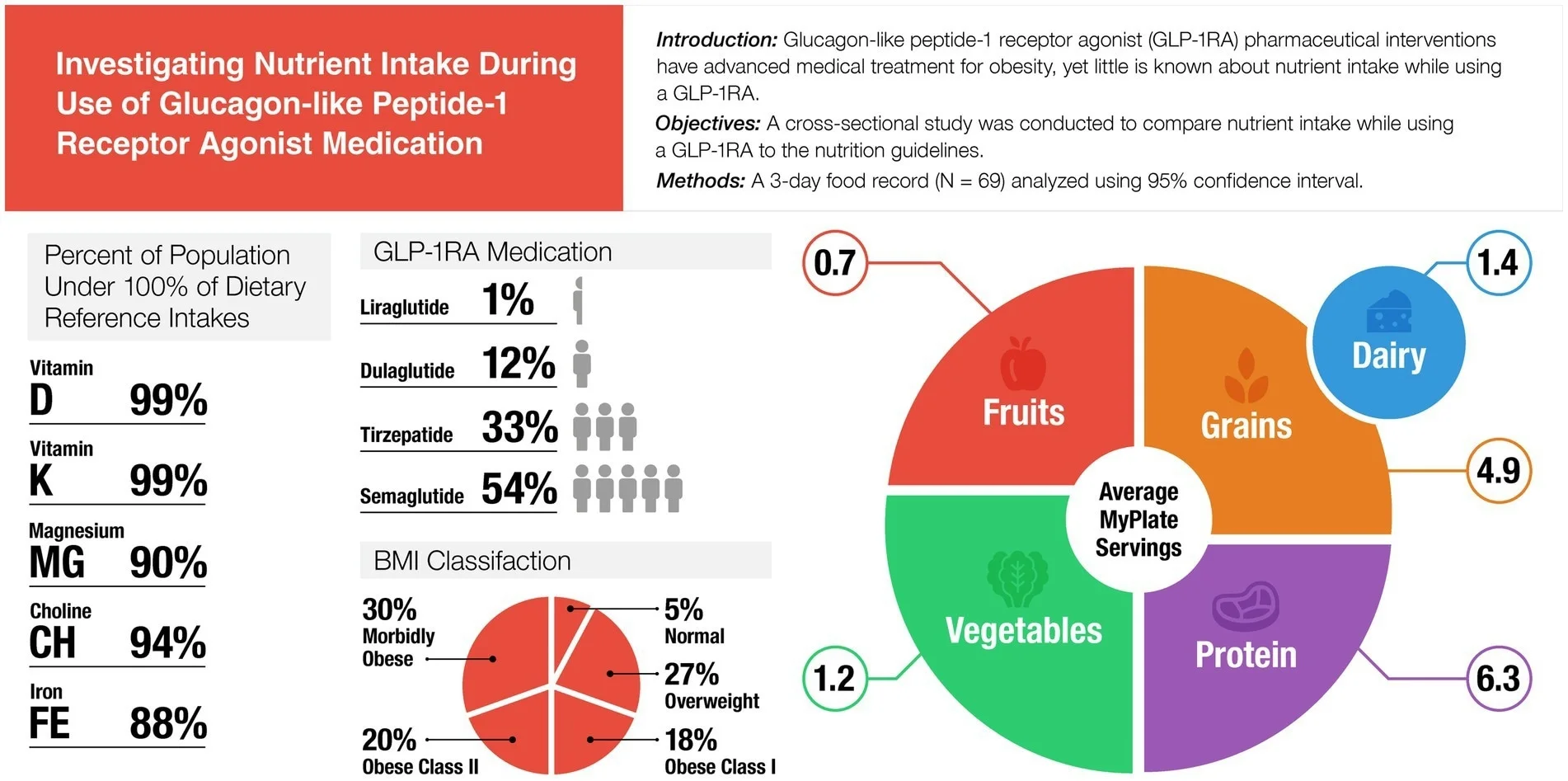
The number that spread fastest was the 60% regain figure, and it is easy to understand why. It is vivid, simple, and emotionally powerful. Patients who hear that figure may immediately fear that stopping treatment means nearly all their effort will be undone. That fear is understandable, but the study’s actual message is slightly more careful. The regain estimate refers to the proportion of weight lost during treatment that was later regained, not to a complete return to baseline body weight in every person. Some people regained more, some less, and the overall trend varied across studies.
Still, the figure matters because it confirms what clinicians have increasingly suspected from practice. Weight regain after stopping GLP-1 medications is common, not rare. That pattern is consistent with a broader 2025 meta analysis also published in eClinicalMedicine, which found that discontinuation of GLP-1 receptor agonists in adults with obesity was associated with significant metabolic rebound, including body weight gain, worsening HbA1c, higher fasting plasma glucose, larger waist circumference, and increased systolic blood pressure.
This is one reason the review landed so heavily in public discussion. It took a feeling many people already had and gave it stronger numbers. Patients who stop these drugs do not just face psychological difficulty keeping weight off. They may also face biological pressure toward regain, with appetite, metabolic signaling, and weight regulation mechanisms shifting again once the medication is withdrawn. Experts quoted by the Science Media Centre noted that this pattern fits what is already known about obesity as a chronic relapsing condition rather than a simple failure of willpower.
What the study actually looked at
One reason this review has attracted both praise and caution is the breadth of the included evidence. The paper examined 48 studies involving adults who were overweight, obese, or living with conditions such as diabetes. The participants did not all start from the same place, use the same drugs, stay on treatment for the same length of time, or stop medication under the same circumstances. Some studies involved liraglutide, while others looked at semaglutide or tirzepatide. Some populations had kidney disease or diabetes. Others were being treated primarily for obesity.
That diversity is both a strength and a limitation. It gives the review broad relevance across real world clinical populations, but it also means the estimates are averages drawn from very different groups. ABC News medical correspondent Dr. Tara Narula highlighted this point when discussing the review, noting that the wide range of participants and treatment conditions means the conclusions should not be applied rigidly to every patient. She emphasized that weight loss requires an individualized approach, because some people may be able to come off the drugs and maintain results, while others may need tapering or even indefinite treatment.
That individual variation may ultimately be one of the most important takeaways. A review like this gives a clearer map of the average trajectory, but it cannot predict exactly what will happen to any one person. It can warn patients and doctors that regain is common. It cannot tell them with certainty who will keep more weight off, who will benefit from a lower maintenance dose, or who may need ongoing therapy to preserve metabolic gains.
Why GLP-1 drugs work so well in the first place

Part of the intensity around this review comes from how transformative these medications have seemed. GLP-1 receptor agonists and related drugs help regulate appetite, slow gastric emptying, improve satiety, and in many patients substantially reduce caloric intake. Clinical and real world evidence has shown that they can produce average weight loss on a scale that lifestyle programs alone often struggle to achieve. The Cambridge summary noted that patients often lose around 15% to 20% of body weight on these drugs, a range that has reshaped expectations for non surgical obesity treatment.
That success is precisely why the question of stopping is so important. When a treatment produces large losses, any rebound will look dramatic. The review also found that the amount of weight regained tended to be proportional to the amount originally lost. In other words, the greater the initial success, the more visible the rebound may be after discontinuation. That does not mean successful weight loss is a mistake. It means maintenance planning becomes even more crucial when treatment works especially well.
This is also why simplified public debate can become misleading. Some critics of GLP-1 drugs point to rebound as proof the medications are not worth it. Some enthusiasts treat them as if they solve obesity permanently. The truth emerging from the evidence is more complicated. These medications can be highly effective, but that effectiveness does not eliminate the chronic biology of obesity once treatment stops.
The part patients may find most discouraging
Perhaps the hardest part of the new findings is emotional rather than statistical. Many patients who use GLP-1 medications have already spent years struggling with weight, dieting, exercise programs, shame, and frustration. For them, successful weight loss is often about far more than appearance. It can mean better mobility, reduced pain, lower blood sugar, improved fertility, and a profound sense of relief. To hear that much of that weight may return after stopping treatment can feel like another cycle of hope followed by disappointment.
But the review does not actually say that patients are doomed to fail. It says that the average trajectory after stopping medication is unfavorable unless there is a strategy to support maintenance. That distinction matters. The message is not “there is no point.” The message is “do not assume the job is finished when the prescription ends.” That is a more difficult message, but also a more useful one.
Dr. Tara Narula underscored another important point on ABC News. Even with regain, not all the lost weight came back. She said the maintained reduction from baseline was around 4% to 5%, and that such a result is not clinically insignificant. In medicine, modest sustained changes often matter more than public conversation admits. They may not satisfy dramatic expectations, but they can still improve long term health.
Could tapering help reduce regain

One of the most intriguing parts of the current discussion is whether stopping these medications abruptly may be part of the problem. Narula noted that some data suggest a dose tapering strategy, gradually lowering the dose over time, might help prevent or reduce weight regain. That does not yet amount to a universal rule, and the current evidence is not strong enough to declare tapering the answer for everyone. But it does point toward a more realistic future model of care, one in which discontinuation is treated as an active clinical process rather than a sudden off switch.
Experts responding through the Science Media Centre also stressed that the paper does not prove everyone should remain on these medications indefinitely. Some specialists said it reinforces the idea that obesity, like hypertension or diabetes, often requires long term management, but they also emphasized that medication decisions must balance benefits, side effects, cost, and patient preference.
This matters especially because real world discontinuation rates are high. Cambridge researchers noted that cost and side effects contribute to many patients stopping within a year. So even if long term maintenance dosing turns out to help many people, the question will remain whether health systems, insurers, and patients can realistically sustain that model over time.
Why lifestyle support still matters
The new review does not diminish the role of lifestyle interventions. In fact, it may make them more important. Narula emphasized that counseling, exercise, nutrition changes, and in some cases additional medications can all help patients lose weight and keep it off over the long term. She also suggested that some people may leave GLP-1 treatment having permanently changed behaviors or even aspects of appetite regulation and brain response, which could help explain why not all lost weight is regained.
This is an area where the public conversation often becomes too binary. It is unhelpful to frame the issue as medication versus lifestyle. For many patients, the more realistic picture is medication plus lifestyle, or medication followed by an intensive maintenance plan. The review supports that broader perspective because it shows that stopping the drug does not erase the value of what was achieved, but it does make continued support essential.
Lifestyle treatment alone is often difficult, especially for people with severe obesity or diabetes related complications. But lifestyle treatment after successful GLP-1 use may function differently than lifestyle treatment before it. A patient who has already lost meaningful weight may move more easily, sleep better, feel more motivated, and experience fewer physical barriers to exercise and healthier habits. That possibility may help explain why some weight loss is maintained even after stopping medication.
What this means for the future of obesity care
The biggest implication of this review is that obesity treatment is moving further away from the fantasy of a one time fix. The evidence increasingly suggests that for many patients, successful weight management will require a long horizon, flexible treatment plans, and honest discussion about what happens after the initial weight loss phase. That may include maintenance dosing, slower tapering, additional medications, structured behavioral support, or some combination of all four.
In that sense, the review may actually improve patient care by setting more realistic expectations. Hope is important, but false simplicity is not. People deserve to know that these drugs can help substantially, and they also deserve to know that stopping them may bring back much of the lost weight unless there is a thoughtful plan in place. That is not a reason to reject the medications. It is a reason to treat them with the seriousness of long term therapy rather than the hype of a quick trend.
The review also raises a broader social question. If obesity is increasingly understood as a chronic disease that often requires sustained treatment, then systems built around short term prescriptions and patchy insurance coverage may be badly mismatched to the science. Patients may not just need access to GLP-1 drugs. They may need access to continuity. And continuity, in medicine, is often where the real outcomes are decided.
In the end, this new GLP-1 review reveals something both sobering and useful. Yes, many patients regain a substantial portion of lost weight after stopping treatment. But the deeper lesson is not that the drugs disappoint. It is that obesity remains biologically persistent, clinically complex, and highly individualized. The real breakthrough may not be learning that weight can return. It may be learning that the future of treatment depends on planning for that possibility from the very beginning.