Table of Contents
- What Is the Blood-Brain Barrier?
- The Role of the Blood-Brain Barrier in Alzheimer’s Disease
- Targeting 15-PGDH to Protect the Blood-Brain Barrier
- Benefits of Protecting the Blood-Brain Barrier
- Early Success in Animal Models
- Challenges and Future Directions
- A Shift in Alzheimer’s Treatment
- The Promise of a Breakthrough Treatment
- A New Hope for Alzheimer’s Patients
What Is the Blood-Brain Barrier?
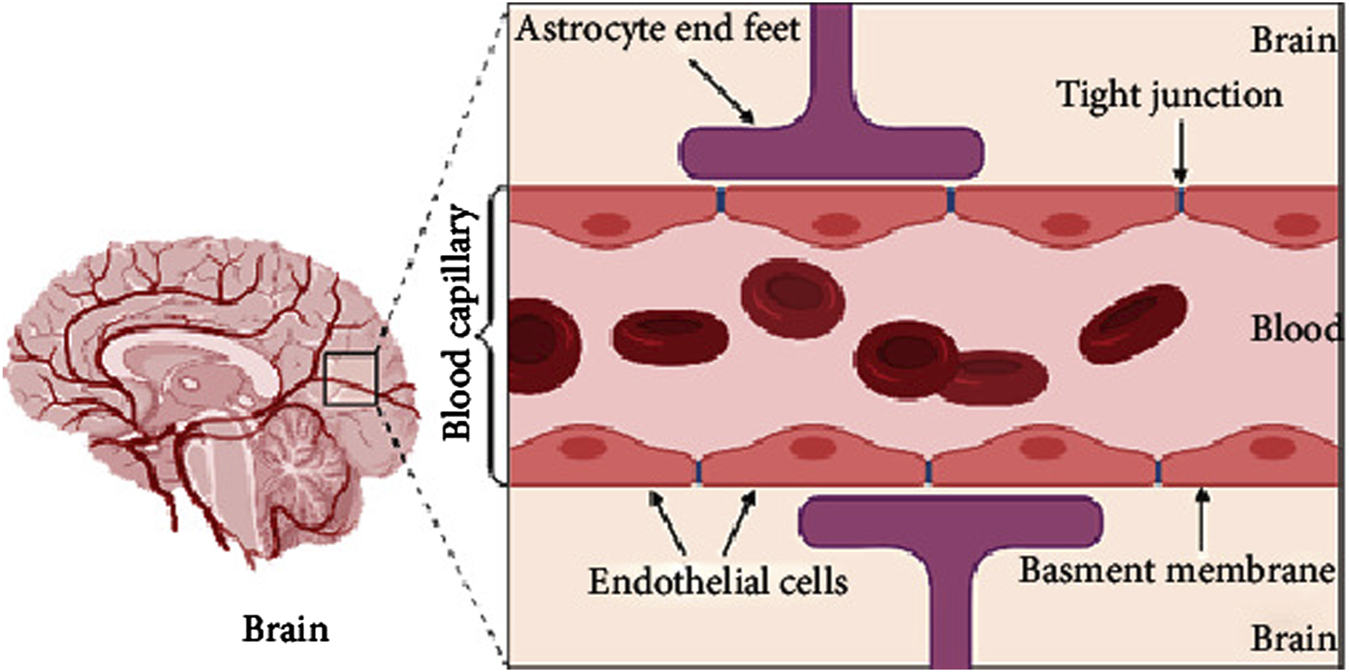
The blood-brain barrier (BBB) is one of the most sophisticated defense mechanisms in the human body. Composed of tightly connected cells lining the blood vessels in the brain, the BBB controls which substances can pass from the bloodstream into the brain. This barrier allows essential nutrients and molecules to enter while blocking harmful toxins, pathogens, and other potentially damaging substances. In essence, the BBB acts as a fortress, protecting the brain from a wide array of potential threats.
When the BBB is functioning properly, it ensures that the brain remains shielded from harmful invaders, such as bacteria or viruses, while allowing necessary nutrients and oxygen to reach brain cells. However, as Alzheimer’s disease progresses, the BBB begins to weaken. This breakdown of the barrier allows harmful molecules to infiltrate the brain, triggering inflammation and damaging brain cells. Over time, this damage contributes to the cognitive decline seen in Alzheimer’s patients.
The Role of the Blood-Brain Barrier in Alzheimer’s Disease
Recent research has increasingly pointed to the BBB’s role in Alzheimer’s disease. The breakdown of this protective barrier is one of the earliest events in the disease process, often occurring before other hallmark signs, such as amyloid plaque buildup, are evident. When the BBB becomes compromised, harmful molecules and inflammatory cells can enter the brain, triggering a cascade of damaging responses that contribute to neuronal death and cognitive decline.
Scientists have discovered that in addition to amyloid plaques and tau tangles, BBB dysfunction plays a significant role in the progression of Alzheimer’s. As the barrier weakens, the brain becomes more vulnerable to inflammation, oxidative stress, and the accumulation of toxic substances. This sets the stage for the neurodegeneration that leads to the memory loss and cognitive impairments characteristic of the disease.
Targeting 15-PGDH to Protect the Blood-Brain Barrier
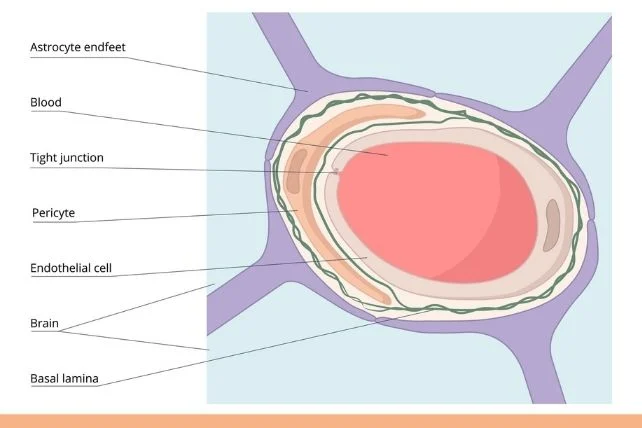
A new drug in development aims to prevent the breakdown of the BBB by targeting an enzyme known as 15-hydroxyprostaglandin dehydrogenase (15-PGDH). This enzyme, which is involved in the regulation of inflammatory responses, has been found to play a key role in the breakdown of the BBB. By inhibiting 15-PGDH, researchers hope to protect the barrier, reduce brain inflammation, and slow the progression of Alzheimer’s disease.
Studies have shown that in patients with Alzheimer’s, 15-PGDH activity is abnormally high. This enzyme is concentrated in cells surrounding the blood-brain barrier, and its activity contributes to the weakening of the BBB. By blocking 15-PGDH, scientists can potentially prevent the loss of the protective barrier, thereby protecting the brain from the harmful effects of inflammation and oxidative stress.
In laboratory studies, the inhibition of 15-PGDH has shown promising results. In animal models of Alzheimer’s, the drug successfully preserved the integrity of the BBB, reduced inflammation, and improved cognitive function. These findings suggest that targeting 15-PGDH could be a viable therapeutic strategy for slowing or even halting the progression of Alzheimer’s disease.
Benefits of Protecting the Blood-Brain Barrier
The primary benefit of protecting the blood-brain barrier in Alzheimer’s patients is the potential to slow or prevent the cognitive decline that is characteristic of the disease. By preserving the integrity of the BBB, researchers believe that it may be possible to keep harmful substances out of the brain, reduce inflammation, and protect neurons from damage. This could ultimately delay the onset of symptoms and improve the quality of life for those affected by Alzheimer’s.
In addition to slowing the progression of Alzheimer’s, protecting the BBB may also help to alleviate some of the secondary symptoms associated with the disease, such as mood swings, anxiety, and sleep disturbances. By addressing the root cause of much of the brain’s vulnerability, this approach could offer a more comprehensive treatment option than current therapies, which primarily focus on alleviating symptoms rather than stopping the underlying damage.
Early Success in Animal Models
The experimental drug targeting 15-PGDH has already shown promising results in animal models of Alzheimer’s. In these studies, mice with Alzheimer’s-like symptoms were treated with the drug, which resulted in significant improvements in cognitive function. In memory tests, the treated mice performed much better than untreated mice, showing that the drug had successfully preserved their brain function.
One of the most striking findings was that the treated animals exhibited less inflammation in the brain, a key factor in Alzheimer’s progression. Additionally, the drug helped to maintain the integrity of the blood-brain barrier, preventing the leakage of harmful substances into the brain. This provided a clear indication that the drug could be effective in humans, offering new hope for a disease that has proven resistant to many existing treatments.
Challenges and Future Directions

While the results in animal models are encouraging, much more research is needed before this therapy can be applied to humans. One of the main challenges is ensuring that the drug can be safely and effectively administered to patients. In particular, researchers must ensure that the drug can reach the brain without causing unwanted side effects.
Another challenge is determining how long the effects of the drug will last. Although the drug has shown promising results in the short term, it will be essential to test its long-term efficacy in clinical trials. If the drug can continue to protect the blood-brain barrier and prevent cognitive decline over extended periods, it could become a game-changer in the treatment of Alzheimer’s disease.
A Shift in Alzheimer’s Treatment
The development of this new drug marks a significant shift in Alzheimer’s research. For years, scientists have focused on amyloid plaques and tau tangles as the primary targets for treatment. However, the new approach of protecting the blood-brain barrier offers a novel way to address the disease’s underlying causes. By focusing on preserving the brain’s defenses rather than attacking the plaques directly, this strategy could offer a more comprehensive solution to Alzheimer’s.
This shift in focus could also open the door to new treatments for other neurodegenerative diseases. Conditions such as Parkinson’s disease, multiple sclerosis, and traumatic brain injury are all associated with inflammation and BBB dysfunction. By protecting the blood-brain barrier, researchers may be able to slow the progression of these diseases as well.
The Promise of a Breakthrough Treatment
As research on this new drug continues, the potential for a breakthrough treatment for Alzheimer’s grows. If the drug proves effective in human trials, it could represent a major advancement in the fight against Alzheimer’s and other neurodegenerative diseases. By targeting the blood-brain barrier and reducing inflammation, this approach could slow the progression of the disease, improve quality of life, and provide a new path forward for Alzheimer’s treatment.
A New Hope for Alzheimer’s Patients
The development of a drug that protects the blood-brain barrier and reduces inflammation offers a new hope for patients with Alzheimer’s disease. By focusing on preserving the brain’s defenses rather than targeting the amyloid plaques directly, this approach could provide a more effective and comprehensive treatment option. While much work remains to be done before this drug becomes widely available, the early success in animal models is a promising sign that we are one step closer to finding a cure for Alzheimer’s.
As the research progresses, we may soon see a shift in the way Alzheimer’s is treated, with therapies that focus on preventing the disease’s onset rather than simply managing its symptoms. This could mark a new era in Alzheimer’s treatment, offering patients and their families the hope of a brighter, more independent future.